159 North 3rd Street
Macclenny, Florida 32063

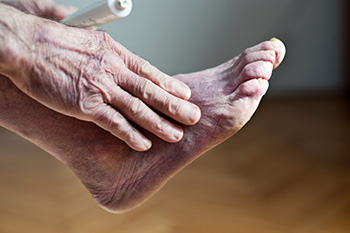 Poor circulation can cause various signs and symptoms that suggest a problem with blood flow. Some of the most common symptoms include cold or numb feet and toes, which can make the feel unusually cold to the touch. You might also experience tingling or a “pins and needles” sensation. Additional symptoms of poor circulation include swelling in the lower legs and feet, as well as changes in skin color, such as turning pale or blue. Poor circulation can contribute to cramping or pain in your legs and feet, especially after physical activity. One common cause of poor circulation is atherosclerosis, where fatty deposits build up in your arteries, narrowing them and restricting blood flow. Symptoms may include chest pain, shortness of breath, and fatigue, usually while participating in physical activity. Regular check-ups and a healthy lifestyle can help manage and prevent atherosclerosis. If you notice any of these symptoms of poor circulation in the feet, it's suggested that you consult with a podiatrist to address the issue.
Poor circulation can cause various signs and symptoms that suggest a problem with blood flow. Some of the most common symptoms include cold or numb feet and toes, which can make the feel unusually cold to the touch. You might also experience tingling or a “pins and needles” sensation. Additional symptoms of poor circulation include swelling in the lower legs and feet, as well as changes in skin color, such as turning pale or blue. Poor circulation can contribute to cramping or pain in your legs and feet, especially after physical activity. One common cause of poor circulation is atherosclerosis, where fatty deposits build up in your arteries, narrowing them and restricting blood flow. Symptoms may include chest pain, shortness of breath, and fatigue, usually while participating in physical activity. Regular check-ups and a healthy lifestyle can help manage and prevent atherosclerosis. If you notice any of these symptoms of poor circulation in the feet, it's suggested that you consult with a podiatrist to address the issue.
Poor circulation is a serious condition and needs immediate medical attention. If you have any concerns with poor circulation in your feet contact Dr. John L. Coleman of Florida. Our doctor will treat your foot and ankle needs.
Poor Circulation in the Feet
Poor blood circulation in the feet and legs is can be caused by peripheral artery disease (PAD), which is the result of a buildup of plaque in the arteries.
Plaque buildup or atherosclerosis results from excess calcium and cholesterol in the bloodstream. This can restrict the amount of blood which can flow through the arteries. Poor blood circulation in the feet and legs are sometimes caused by inflammation in the blood vessels, known as vasculitis.
Causes
Lack of oxygen and oxygen from poor blood circulation restricts muscle growth and development. It can also cause:
Those who have diabetes or smoke are at greatest risk for poor circulation, as are those who are over 50. If you have poor circulation in the feet and legs it may be caused by PAD and is important to make changes to your lifestyle in order to reduce risk of getting a heart attack or stroke. Exercise and maintaining a healthy lifestyle will dramatically improve conditions.
As always, see a podiatrist as he or she will assist in finding a regimen that suits you. A podiatrist can also prescribe you any needed medication.
If you have any questions please feel free to contact our office located in Macclenny, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
The purpose of the body’s circulation system is to transport blood, oxygen, and nutrients throughout the body. A reduction of blood to a specific part of the body may cause one to experience symptoms of poor circulation. The most common causes of poor circulation in the feet are obesity, diabetes, and heart conditions such as peripheral artery disease (PAD). Common symptoms of poor circulation include tingling, numbness, throbbing, pain and muscle cramps.
Peripheral artery disease is a common cause of poor circulation in the legs. Symptoms of PAD are cramping, pain or tiredness in the leg or hip muscles while walking or climbing stairs. This pain tends to go away with rest and starts back up when you begin to walk. It is a condition that causes the blood vessels and arteries to become narrow. Although PAD is more common in adults over the age of 50, it may also occur in younger people. A similar condition called atherosclerosis causes arteries to stiffen up due to a buildup of plaque in the arteries and blood vessels.
Blood clots are also a common cause of poor circulation in the feet. Clots may obstruct blood vessels and if they occur in the legs, they may eventually lead to pain and discoloration. This occurrence is commonly known as deep vein thrombosis (DVT) and it may travel to the lungs. Varicose veins are another condition that may lead to poor circulation, and it is caused by incompetence of the valves in the veins. Women who are overweight are prone to developing this condition. Lastly, diabetes, which is correlated with poor blood sugar metabolism may lead to chronic poor circulation. Those with diabetes often suffer from cramping in the legs, calves, thighs and buttocks.
If you are looking for ways to avoid poor circulation there are some tips you can follow. One tip is to avoid sitting for too long. If you plan to sit down for a long period of time, you should try standing up occasionally, to improve your circulation. Another great way to avoid poor circulation is to exercise. Exercise is an excellent way to pump the heart and increase blood flow. Those who suffer from poor circulation should also avoid smoking, reduce their salt intake, and try to lose weight.
If you are experiencing symptoms from poor circulation in your feet, you should consult with your podiatrist to determine the best method for treatment for you. He or she may prescribe medication in addition to recommending specific lifestyle changes to improve your circulation.
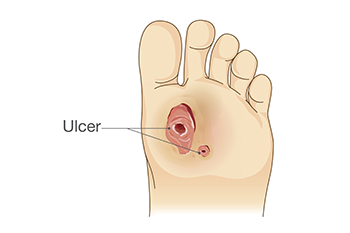 Foot ulcers are a serious concern for individuals with diabetes. Ulcers in the lower extremities are caused by many factors, including nerve damage and poor circulation. These are common complications of diabetes. When a wound or sore develops on the foot, decreased feeling caused by neuropathy can make it difficult to notice. This can lead to delays in treatment and allow time for the wound to worsen. On top of that, impaired circulation interferes with the body's ability to heal, causing diabetic foot ulcers to heal more slowly and become more prone to infection. Without proper care, diabetic foot ulcers can become severe, potentially leading to serious problems such as tissue damage and even amputation. Diabetics need to prioritize foot care as part of their management plan. This includes daily foot inspections, appropriate footwear, maintaining blood sugar levels, and seeking immediate medical attention for any foot complications. Podiatrists play an important role in managing diabetic foot ulcers with specialized care and treatment to promote healing and prevent further complications. If you have developed a diabetic foot ulcer, it is suggested that you visit a podiatrist immediately for an exam and treatment.
Foot ulcers are a serious concern for individuals with diabetes. Ulcers in the lower extremities are caused by many factors, including nerve damage and poor circulation. These are common complications of diabetes. When a wound or sore develops on the foot, decreased feeling caused by neuropathy can make it difficult to notice. This can lead to delays in treatment and allow time for the wound to worsen. On top of that, impaired circulation interferes with the body's ability to heal, causing diabetic foot ulcers to heal more slowly and become more prone to infection. Without proper care, diabetic foot ulcers can become severe, potentially leading to serious problems such as tissue damage and even amputation. Diabetics need to prioritize foot care as part of their management plan. This includes daily foot inspections, appropriate footwear, maintaining blood sugar levels, and seeking immediate medical attention for any foot complications. Podiatrists play an important role in managing diabetic foot ulcers with specialized care and treatment to promote healing and prevent further complications. If you have developed a diabetic foot ulcer, it is suggested that you visit a podiatrist immediately for an exam and treatment.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Dr. John L. Coleman from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our office located in Macclenny, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetes can cause two problems that can potentially affect the feet: Diabetic neuropathy and Peripheral Vascular Disease. Diabetic neuropathy occurs when nerves in your legs and feet become damaged, which prevents you from feeling heat, cold, or pain. The problem with diabetic neuropathy is that a cut or sore on the foot may go unnoticed and the cut may eventually become infected. This condition is also a main cause of foot ulcers. Additionally, Peripheral vascular disease also affects blood flow in the body. Poor blood flow will cause sores and cuts to take longer to heal. Infections that don’t heal do to poor blood flow can potentially cause ulcers or gangrene.
There are certain foot problems that are more commonly found in people with diabetes such as Athlete’s foot, calluses, corns, blisters, bunions, foot ulcers, ingrown toenails, and plantar warts. These conditions can lead to infection and serious complications such as amputation. Fortunately, proper foot care can help prevent these foot problems before they progress into more serious complications.
Each day you should wash your feet in warm water with a mild soap. When you finish washing your feet, dry them carefully especially between your toes. You should also perform daily foot inspections to ensure you don’t have any redness, blisters, or calluses. Furthermore, if you are diabetic, you should always wear closed-toed shoes or slippers to protect your feet. Practicing these tips will help ensure that your feet are kept healthy and away from infection.
If you have diabetes, contact your podiatrist if you have any of the following symptoms on your feet: changes in skin color, corns or calluses, open sores that are slow to heal, unusual and persistent odor, or changes in skin temperature. Your podiatrist will do a thorough examination of your feet to help treat these problematic conditions.
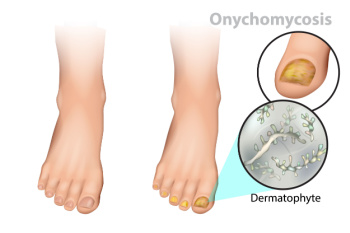
Toenail fungus often develops in distinct stages, progressing gradually if left untreated. Initially, it may appear as a small white or yellow spot under the nail tip. As the infection advances, the nail may thicken and take on a yellowish hue, spreading deeper into the nail bed. Without intervention, the fungus continues its relentless progression, causing the nail to become brittle and crumble at the edges. As the infection worsens, the nail may darken in color, emitting a foul odor, and detachment from the nail bed becomes a possibility. This advanced stage not only affects the appearance of the nail but also brings discomfort and potential complications. Recognizing the signs early on is essential for effective treatment. Consulting a podiatrist for proper diagnosis and guidance is necessary to halt the progression and prevent further damage. If you notice toenail fungus developing, it is suggested that you visit a podiatrist who can prescribe medication for a complete healing.
For more information about treatment, contact Dr. John L. Coleman of Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact our office located in Macclenny, FL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Toenail fungus is a frustrating problem that affects many people. It can be persistent and hard to get rid of. As many different types of fungi are present throughout the environment, it is very easy to contract toenail fungus.
The feet are especially susceptible to toenail fungus because shoes and socks create the ideal dark and moist environment that fungal infections thrive in. While fungal infections of the nail plate are quite common, if left untreated they can spread beyond the toenail and into the skin and other parts of the body.
Signs of toenail fungus include a thickened nail that has become yellow or brown in color, a foul smell, and debris beneath the nail. The toe may become painful due to the pressure of a thicker nail or the buildup of debris.
Treatment for toenail fungus is most effective during the early stages of an infection. If there is an accumulation of debris beneath the nail plate, an ingrown nail or a more serious infection can occur. While each treatment varies between patients, your podiatrist may prescribe you oral medications, topical liquids and creams, or laser therapy. To determine the best treatment process for you, be sure to visit your podiatrist at the first signs of toenail fungus.
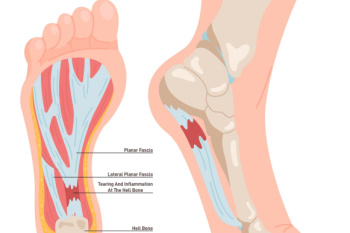
Plantar fasciitis is a foot condition characterized by inflammation and degeneration of the plantar fascia, a thick band of tissue that runs along the bottom of the foot, connecting the heel to the toes. This condition often develops gradually over time, resulting from repetitive strain and stress on the plantar fascia. Activities that involve prolonged standing, walking, or running, especially on hard surfaces, can worsen the problem. Additionally, factors such as obesity, tight calf muscles, high arches, flat feet, and non-supportive footwear can increase the risk of developing plantar fasciitis. Symptoms include heel pain, particularly in the morning or after periods of inactivity, which can worsen with activity. While plantar fasciitis can be challenging to manage, various treatment options, including rest, stretching exercises, orthotic devices, and in severe cases, corticosteroid injections or surgery, can help alleviate pain and promote healing. If you have persistent heel pain, it is strongly suggested that you consult a podiatrist who can accurately diagnose and treat the cause.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. John L. Coleman from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact our office located in Macclenny, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.
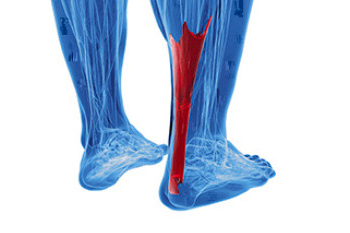
Achilles tendonitis is an ailment affecting the long tendon that connects the leg bones to the heel. This condition is particularly common among those engaged in high-impact activities, like running and jumping. The Achilles tendon's susceptibility to inflammation due to repetitive stress often leads to microtears and thickening. This results in Achilles tendonitis, which is characterized by posterior ankle pain and stiffness. However, the more severe consequence, an Achilles tendon rupture, typically occurs during forceful movements which result in sudden, intense pain and the inability to bear weight. Approximately 80 percent of Achilles tendon ruptures result in complete loss of function in the calf muscle. If you are experiencing pain in the Achilles tendon, it is suggested that you cease the activity causing the pain and make an appointment with a podiatrist as soon as possible. This foot doctor can conduct a thorough exam and determine the appropriate treatment.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Dr. John L. Coleman of Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
Rupture Symptoms
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
If you have any questions please feel free to contact our office located in Macclenny, FL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.